
CPR ventilations are a critical part of CPR and keeping people from passing away.
When a cardiac arrest even occurs, it will typically be managed through a combination of airway and ventilation techniques in an attempt to administer cardiopulmonary resuscitation. These combined processes are typically what the term “CPR” refers to.
While the “best” combination of airway techniques, oxygenation, and ventilation is still not entirely clear, there are standard practices to follow based on the best available knowledge we have.
Unfortunately, even the most cutting-edge research into advanced cardiopulmonary resuscitation (CPR) have only led to slight improvements in cardiac arrest patients’ outcomes, and the use of ventilations in CPR is one of the most uncertain areas of knowledge.
That said, current evidence gathered from observational studies and randomised controlled trials indicate that a stepwise approach to airway management adjusted to the needs of the patient and the skills of the rescuer during resuscitation is best.
The person performing CPR should always prioritise delivering the maximum amount of oxygen possible to the patient and, if possible, using waveform capnography once an advanced airway is in place.
How often should you provide ventilations in CPR?
When providing CPR ventilations to an adult, 1 ventilation should be given roughly every 5 seconds.
When providing CPR ventilations to a child, 1 ventilation should be given roughly every 3 seconds.
What is the Correct CPR Ventilation/Compression Ratio?
Remember that for adults the correct ventilation/compression ratio is 30:2, which just means that 2 rescue breaths should be provided after 30 compressions, and this should be done in a steady rhythm.
And what is the CPR Ventilation/Compression Ratio for infants and children?
For children and babies, the ventilation/compression ratio is 15:2, so 2 rescue breaths for every 30 compressions.
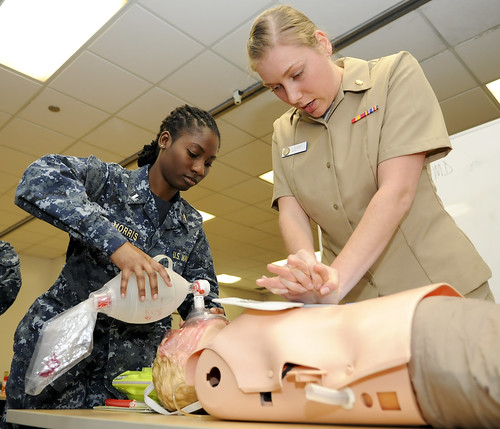
HOW TO GIVE VENTILATIONS IN CPR USING A BAG-VALVE-MASK RESUSCITATOR (TWO
RESCUERS)
If there are two rescuers available, you should perform two-rescuer CPR. One of you will handle ventilations while the other takes care of chest compressions.
- After briefly but carefully assessing the scene for safety (making sure there is no risk of fire, for example), you can then do a primary assessment. During the primary assessment, prepare the bag-valve-mask resuscitator (BVM), making sure that you’ve chosen an appropriate size for the patient.
- If the patient has a pulse but is not breathing, rescuer 1 should position the mask over the cardiac arrest victim’s mouth and nose while kneeling behind their head.
- Rescuer 1 should seal the mask.
- Rescuer 1 should proceed to open the airway by:
Placing their thumbs along each side of the mask, supporting the operation with their elbows.
Sliding their fingers behind the angles of the victim’s jawbone.
Pushing down on the mask with the thumbs, lifting the jaw and tilting the head back. - Rescuer 2 now begins with the ventilations by squeezing the bag slowly with both hands.
For an adult, 1 ventilation should be given roughly every 5 seconds.
For a child, 1 ventilation should be given roughly every 3 seconds.
Important: Each ventilation should last about 1 second and make the chest clearly rise. The chest should fall before the next ventilation is given. - Rescuer 2 should check for breathing and a pulse every two minutes by removing the mask, looking, listening, and feeling for breath and a pulse. Do not do this for any longer than 10 seconds before resuming ventilations if no breath is detected.
If the victim is unconscious and there is no breathing or pulse – immediately begin performing CPR. Ventilations are only for victims who are unconscious, have a pulse, but are breathing – otherwise they need CPR.
If the victim is unconscious but breathing, place them in the recovery position.
After performing the first steps of CPR, it’s very important to ensure that the patient is getting enough oxygen and that CO2 washout is also sufficient through doing CPR ventilations.
