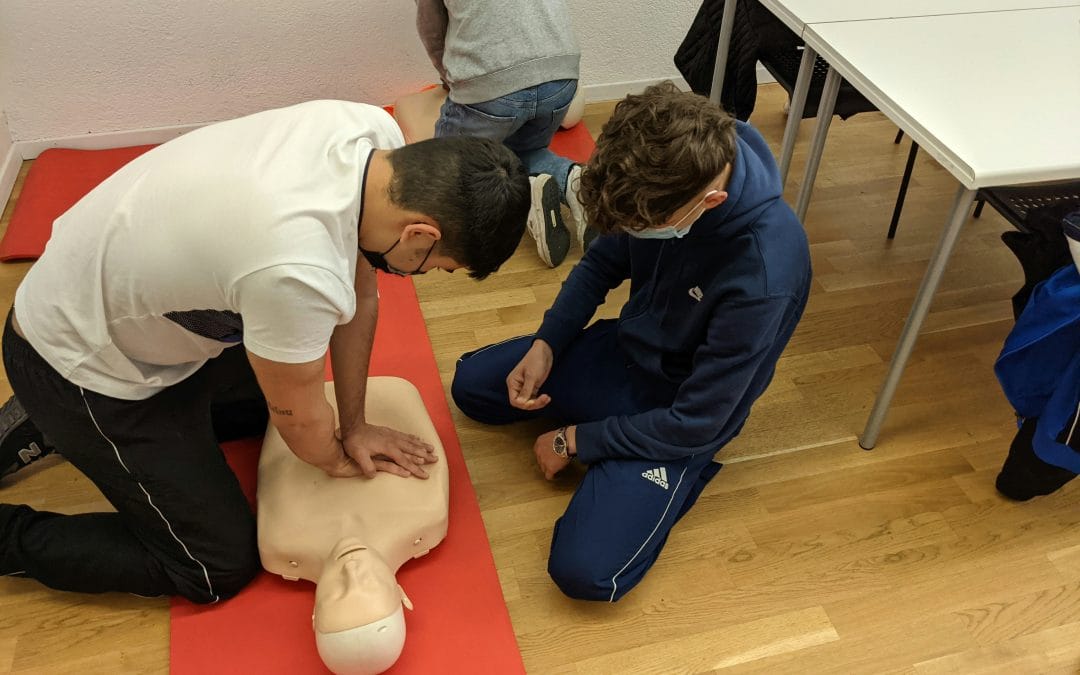
First aid and CPR are often taught as a set of physical actions that must be performed quickly and correctly. While those skills remain essential, every emergency also unfolds within a powerful emotional space. Fear, uncertainty, and urgency can shape how people think and move in those first critical moments.
A responder may know the steps by heart, yet still struggle to act if their mind feels overwhelmed. Mental health awareness raises awareness of this hidden layer of emergency care.
It helps explain why some people hesitate, why others rush in, and how calm communication can change the direction of a tense situation. Recognizing the emotional side of emergencies allows responders to offer care that supports both the body and the mind.
How Stress Shapes Human Reactions in Emergencies
When an emergency unfolds, the brain shifts into a survival mode. Heart rate rises, breathing becomes shallow, and attention narrows. These changes can help a person act quickly, but they can also create mental blocks. Some people struggle to recall even simple steps they practiced before.
Medical emergencies can increase stress for both care recipients and providers. A study found that many patients undergoing surgery because of a medical emergency feel stressed. This weakens their immune function and increases the risk of complications. Among 309 patients, about one-third experienced significant stress, which was linked to lower white blood cell and lymphocyte counts.
Responders without ample experience can also feel this stress. Mental health awareness helps responders recognize these reactions in themselves. It reminds them that stress is a normal response, not a sign of failure. This understanding can reduce self-criticism and keep focus on the task at hand.
Recognizing mental health challenges can also enable them to develop coping strategies. A survey notes three main themes for coping: preparing for the most challenging conditions, relying on supportive partnerships, and maintaining balance. These themes included mental preparation and risk management, collaboration and clear communication with others, as well as behaviors that help individuals adapt.
What techniques can responders practice daily to improve their stress tolerance?
Controlled breathing exercises, brief mindfulness sessions, and visualization of calm responses during imagined emergencies can strengthen emotional control. These practices train the nervous system to recover more quickly from sudden stress, which can improve focus and decision-making in real situations.
Recognizing Emotional Cues in Patients and Bystanders
People in medical distress often show signs beyond physical symptoms. Panic, confusion, or withdrawal can appear even before visible injuries.
Bystanders, especially family members, can also face an emotional shock. In fact, a study concluded that out-of-hospital cardiac arrest recognition rates were lower in family members, and emotional stress was presented as a barrier to CPR performance.
Bystanders may even need help from a therapist or social worker to cope with it. According to the University of the Pacific, someone with a master’s in social work (MSW) has empathy, resilience, and adaptability to help bystanders rebuild their lives.
It has become easier to find qualified social workers, as online education offers flexibility and advanced-standing programs enable quick graduation. Someone with a bachelor’s degree can enroll in an advanced standing MSW online program, encouraging more professionals to pursue a career in this field.
A responder who understands basic emotional cues can manage the space more effectively. Simple reassurance can slow a racing breath or ease a tense posture. Clear and steady communication can turn anxious onlookers into helpful allies. These small actions support both emotional stability and physical care.
How can cultural differences affect emotional cues in a medical emergency?
Cultural background can influence how people express fear, pain, or distress. Some may become very vocal, while others may grow quiet and reserved. Understanding these differences helps responders avoid misreading emotional signals. It also supports respectful communication that aligns with the person’s comfort level and expectations.
Training the Mind Alongside the Body
Many training programs focus on muscle memory and procedural accuracy. These elements matter, yet mental readiness deserves equal attention. Courses that address stress management, confidence building, and communication skills prepare learners for the full scope of an emergency.
Volunteer responders should focus on mental preparedness more than traditional, licensed responders. A study notes that volunteer responders are highly motivated to help others. However, they may initially face shock if they are not mentally prepared. This is because they don’t have as much training and experience as professional first responders. In such cases, alerting them beforehand about the situation can help minimize the initial shock.
Sometimes, an incident can affect future readiness and confidence. Understanding trauma responses allows trainers and supervisors to support their teams and volunteers better.
Gentle debriefing sessions can help people process what happened. This can turn a difficult event into a learning experience rather than a lingering burden. Over time, this approach can strengthen both skill retention and emotional resilience.
What role can virtual simulations play in improving mental readiness for emergency response?
Virtual simulations allow learners to experience realistic scenarios without physical risk. These tools can recreate noise, time pressure, and unexpected changes. Exposure to these conditions helps students practice emotional regulation and quick thinking. This type of training can prepare them for the mental demands of real emergencies.
Building a Culture of Awareness in Emergency Training
Organizations that value mental health create safer learning environments. They allow questions about fear, hesitation, and stress without judgment. This openness helps learners practice skills in a supportive, rather than pressure-filled, environment.
Over time, this culture can shape how responders see their role. They begin to view emergencies as human events, not just technical challenges. This perspective can improve patience, clarity, and cooperation during real-world situations.
There’s also a need to raise public awareness. A qualitative study explored how UK ambulance call handlers perceive barriers to initiating CPR during emergency calls. Interviews with 30 call-handlers revealed that strong caller emotions, physical challenges at the scene, and uncertainty about whether CPR was needed were the most common obstacles.
Participants described each call as a unique and often ambiguous situation, especially in care settings. The findings suggest that current protocols may not fully address these complexities and that call-handler insights can guide improvements to CPR instruction and support.
Effective first aid and CPR rely on more than correct technique. They depend on how people think, feel, and connect in moments of crisis. Mental health awareness brings a deeper understanding of these human elements.
It helps responders manage their own stress, support those in distress, and communicate with purpose. When the mind and body work together, the response becomes stronger, steadier, and more compassionate.